Current Views on Lateral Epicondylitis
- Whitney Lowe
Introduction
One of the most common upper extremity overuse problems is lateral epicondylitis (LE), commonly called tennis elbow. LE affects roughly 1 – 3% of the general population in the U.S. each year. Despite its common name of tennis elbow, only about 5% of the people with LE developed the condition from playing tennis.(1) Due to the nature of our work, LE is also a common problem affecting massage therapists.
The dramatic increase in repetitive motions in numerous occupations has led to a surge of epicondylitis over the last several decades. This condition also has heavy socioeconomic burdens, including lost productivity for employers, lost or diminished employee wages, long periods of pain, and significant workers’ compensation claims. This article will focus on lateral epicondylitis, but the same principles hold for medial epicondylitis, a similar condition affecting the wrist flexor muscles.
Anatomical Background
Lateral epicondylitis affects the common wrist extensor tendon near the elbow. This proximal tendon is a conjoined tendon shared by the extensor carpi radialis brevis, extensor digitorum, extensor digiti minimi, and extensor carpi ulnaris (Image 1). The main tendon affected in most cases of LE is the extensor carpi radialis brevis (ECRB).

Extensor carpi radialis brevis
It’s not immediately clear why this tendon is affected more than the others, except that its anatomical arrangement and line of pull are likely putting the greatest load on this portion of the tendon.
This common tendon inserts into the lateral epicondyle of the humerus. When the tendon is overused, tenderness can be felt in the tendon and where it blends into the periosteum of the bone. The periosteum is a thin membrane covering the bone and is one of the most pain-sensitive tissues in the body. That is one reason constant pulling from an overused tendon produces pain at the tendon attachment site.
The Pathology
LE is most commonly associated with repetitive overuse actions of the wrist extensor muscles. These actions could include repetitive or forceful wrist extension, long periods of gripping objects, and movements that include forearm supination or radial deviation. Repetitive eccentric loading on the wrist extensors is also a primary cause. A repetitive eccentric load would be one where the wrist extensors try to prevent the wrist from moving into flexion while slowly resisting that motion (Image 2).
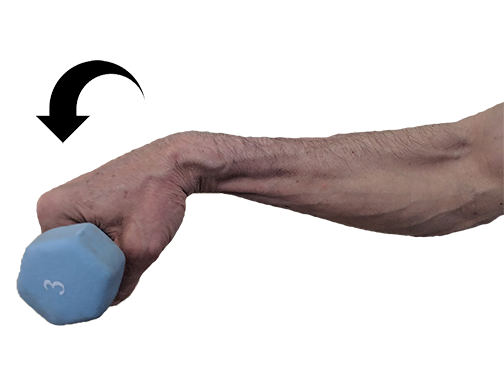
Eccentric loading on the wrist extensor tendons
In addition to repetitive motion, long periods of isometric contraction of the wrist extensors may also lead to LE. For example, grasping tools or implements during occupational activities might not involve repetitive motion as much as a constant contraction to hold the implement in a certain position. For this reason, computer users who spend much time operating a mouse develop epicondylitis. There’s not so much a repetitive wrist extension movement, as the wrist extensors and flexors both engage in chronic isometric activity when holding and manipulating the mouse. Because both muscle groups, flexors and extensors, are overused simultaneously, it is expected to develop either medial or lateral epicondylitis over long periods using a computer mouse.
Other factors play a role in developing epicondylitis. Body mass index, history of rotator cuff disease, de Quervain’s tenosynovitis, carpal tunnel syndrome, and a history of smoking are all correlated with a higher incidence of lateral epicondylitis. It may be that some of these factors developed from the same mechanical stressors and just happened to coincide. The relationship between these corresponding factors is an important distinction. Just because those conditions occur together doesn’t mean one caused the other.
The name of this condition, epicondylitis, would indicate that there is a primary inflammatory component because of its suffix -itis. The original theories of epicondylitis suggested that it resulted from micro-tearing and inflammatory reactions within the extensor tendons. However, further investigations with increasingly sophisticated diagnostic instruments over the last several decades have revealed that epicondylitis, like most chronic overuse tendon disorders, is not an inflammatory condition caused by fiber tearing. Instead, the primary dysfunction appears to be collagen degeneration within the tendon. (2) We have a better understanding of the actual physiology of tendon breakdown in these conditions now, but we still don’t understand why collagen degeneration occurs.
There may still be some minor inflammatory activity at certain stages of the problem. However, framing the condition as one of fiber tearing and inflammation encourages a problematic treatment strategy. One primary treatment method for reducing inflammation in soft tissues is corticosteroid injections. Unfortunately, corticosteroids have detrimental effects on long-term collagen synthesis within soft tissues and are a known factor in tendon weakening. Corticosteroid injections are effective at pain relief, which gives them the impression of healing the condition, but they are detrimental in the long run.
Jill Cook, one of the most prolific researchers into tendon pathology, authored a paper with her colleagues in 2009 that presented a new model for chronic tendon dysfunction such as epicondylitis. (3) This paper proposes that tendon dysfunction exists on a continuum. They have three essential stages of breakdown: reactive tendinopathy, tendon disrepair (failed healing), and degenerative tendinopathy. Each of these different stages has different physiological characteristics and responses to treatment. One reason why many overuse tendon pathology treatments may seem effective is that one treatment is applied to conditions that are at different stages of the continuum. How different treatment strategies match up with the tendon dysfunction continuum is explained further below in the treatment section.
As with other soft tissue pathologies, there is no direct correlation between the amount of pain and the level of tissue degeneration/damage to the tendon. In some cases, there is a significant degree of tissue damage/degeneration with very little pain, while in other cases, there is only a minor degree of damage and a great deal of pain. It is feasible that chronic overuse tendon pain may have more to do with certain biochemical processes in the tissue that irritate nociceptors than a measure of dysfunctional load on the tissues.
Assessment
Identifying lateral epicondylitis is usually pretty straightforward. The tissues are superficial, and the indicators that lead to this are often clearly identified within the client’s history. Initial intake usually reveals some history of repetitive motion or constant isometric load affecting the wrist extensor group. The client may also complain of grip strength loss. Their pain is usually around the lateral aspect of the elbow but may also extend down into the forearm. The pain is commonly described as a dull, aching sensation. Palpating the involved tendons usually increases the pain significantly.
Because the wrist extensor muscles are involved, it seems likely that any motion of active wrist extension should reproduce the pain. However, simply moving the wrist in extension with no additional resistance often does not. Just lifting the wrist has minimal resistance, so very little load is on the tendon in active motion with no additional resistance. If there is resistance throughout the range, reproduction of the client’s pain is more likely.
Pain at the lateral elbow region is also common with resisted wrist extension. The pain is likely even greater if the various extensor tendons are palpated distal to their attachment site during the resisted wrist extension. Palpating the tendon during resisted wrist extension is called the tennis elbow test (Image 3).
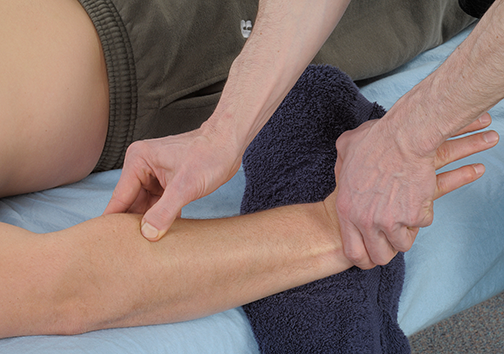
Palpating the wrist tendons during active engagement
Treatment
There is no gold standard treatment for lateral epicondylitis. As noted earlier, the wide variability in treatment effectiveness may be more about the stage of tendon dysfunction than the actual success or failure of a particular treatment approach.
The most common traditional medical treatments for LE are various conservative treatment strategies. Symptoms generally resolve with these conservative treatments within a few months to around a year in some resistant cases. The most common strategies employed include physical therapy, non-steroidal anti-inflammatory drugs (NSAIDs), shockwave therapy, kinesiology taping, biologics, or corticosteroid injections.
Biologics is a general term that refers to several new treatment techniques, such as autologous blood transfusion (collecting blood from the patient and re-transfusing that same blood back into the patient). Platelet-rich plasma (PRP) injection therapy is another approach in this category. PRP injections use a method where platelets, which play a significant role in tissue repair, are extracted from the individual and reinjected to stimulate tissue repair processes. It is also surprising that corticosteroid injections are still used as a treatment strategy even though their potential danger and damage to tendon tissue have been well-documented for decades. They aren’t used anywhere near as often as they used to be, but they are still used in some cases.
The tendon dysfunction continuum model mentioned earlier is divided into two main categories for determining the most effective treatments: reactive tendinopathy and early tendon disrepair, which is the first stage. The second stage is late tendon disrepair and degenerative tendinopathy. Here are some of their recommended treatment strategies at the different stages.
Stage 1:
Pharmacologic interventions like NSAIDS
Tendon load management (reducing the offending load and rest from offending activities)
Stage 2:
Biologic therapies
Shockwave therapy
Exercise (emphasizing eccentric loading on the muscle-tendon unit)
Ultrasound
Massage
So, what role does massage play in epicondylitis treatment? One of the most commonly used massage treatment strategies is deep transverse friction (DTF). Initially, it was thought that the primary benefit of DTF was helping to realign scar tissue from the torn tendon fibers. However, that idea has now fallen out of favor as it has become clear that torn tendon fibers rarely play a role in epicondylitis. Also, it’s unclear whether realigning scar tissue fibers with thumb friction is possible because of the multiple tissues between the thumb and the damaged tissue.
Some research studies that have looked into friction massage have shown that there appears to be some degree of enhanced fibroblast proliferation due to the pressure and movement of the friction massage. So, in LE, pressure and movement on the impaired extensor tendons could encourage the rebuilding of the damaged collagen structure within the tendon.
Another possibility is that friction massage’s critical benefits are not only mechanical (pressure and movement) but also help reduce pain through neurological processes. A neurological principle called conditioned pain modulation (CPM) suggests that, in some instances, a low to moderate pain stimulus can act as a distractor and reduce other pain sensations. (4) Friction massage is usually performed at a level that can be somewhat uncomfortable, so its benefit in pain reduction could be at least partially due to CPM.
An essential aspect of reducing the tendon load to encourage healing is to decrease chronic hypertonicity in the associated muscles. Reducing hypertonicity is another vital role that massage can play in treating epicondylitis. A wide variety of techniques can be effective at helping reduce hypertonicity in the wrist extensor muscles. Superficial applications that appear particularly effective are good compressive effleurage and broad sweeping cross-fiber applications.
As treatment progresses, deeper longitudinal stripping methods are very effective, especially those with a small contact surface like a thumb, fingertip, or pressure tool. Active engagement lengthening techniques appear to bring good results as well. The practitioner applies a deeper longitudinal stripping technique to the wrist extensor muscles while engaged in an eccentric (lengthening) action. Engaging the muscle in an eccentric contraction involves greater neurological input along with the massage technique. This greater neurological input may enhance a pain-reducing process called descending modulation. We know this treatment is particularly effective, and it may be that much of this effect is due to the improved descending modulation.
Lateral epicondylitis can become a debilitating condition. Because it is often related to occupational injuries, it can provoke significant anxiety. It may appear that a person, such as a massage therapist, will no longer be able to continue performing their chosen occupation. When caught early on, activity modification and reduction of the mechanical load can halt the condition’s progression. If it has progressed further, massage is an ideal intervention for enhancing physiological change and managing this common malady’s psychological and social impacts.
Sources
- Lai WC, Erickson BJ, Mlynarek RA, Wang D. Chronic lateral epicondylitis: challenges and solutions. Open Access J Sport Med. 2018;Volume 9:243-251. doi:10.2147/oajsm.s160974
- Bass E. Tendinopathy: Why the difference between tendinitis and tendinosis matters. Int J Ther Massage Bodyw Res Educ Pract. 2012;5(1):14-17.
- Cook JL, Purdam CR. Is tendon pathology a continuum? A pathology model to explain the clinical presentation of load-induced tendinopathy. Br J Sports Med. 2009;43(6):409-416. doi:10.1136/bjsm.2008.051193
- Yarnitsky D. Conditioned pain modulation (the diffuse noxious inhibitory control-like effect): Its relevance for acute and chronic pain states. Curr Opin Anaesthesiol. 2010;23(5):611-615. doi:10.1097/ACO.0b013e32833c348b

