The human hand is critical to our daily activities, especially as massage practitioners. Yet, rarely do we stop and consider what an engineering marvel the hand actually is. The human hand is capable of fine precision movements as well as generating large forces during grasping activities. The skeletal structure of the hand and fingers is a set of rigid bones. Consequently, it takes great muscular control to perform the fine movements of the hand. Without this highly specialized level of control, we would have serious challenges performing all kinds of activities from simply grasping an object to the detailed motor control required to play a musical instrument or perform surgery.
A unique biomechanical pulley system provides the high level of control necessary to move the rigid finger bones with precision. The flexor tendons of the fingers run along the anterior surface of the fingers, and these tendons are tethered close to the bones by connective tissue “pulleys” at eight different locations from the metacarpophalangeal (MCP) joint to the distal phalanx. Because the tendons are closely tethered to the bones, their pulling force is more efficient. Let’s take a look at these pulleys, how they work, and what happens when they don’t.
There are five pulleys in the fingers, called annular pulleys and they are named A1 through A5 (Figure 1).
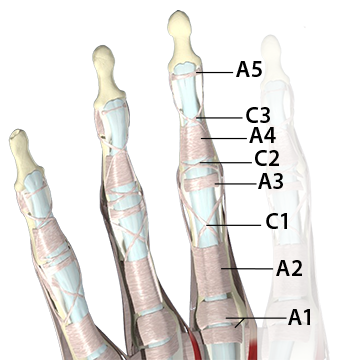
Figure 1: Location of A1 – A5 pulleys
3D anatomy images. Copyright of Primal Pictures Ltd. www.primalpictures.com
The A1, A3, and A5 pulleys are smaller and considered minor pulleys (mostly due to size and not importance). The A2 and A4 pulleys are larger and are sometimes called the major pulleys.1 The A1, A3, and A5 pulleys are located at the MCP, PIP, and DIP joints respectively. The A2 and A4 pulleys are located in the middle of the proximal and middle phalanx respectively (Figure 2).
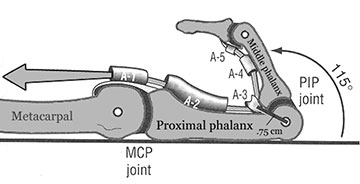
Figure 2: Location of A1 – A5 pulleys
From Neumann, D. A. (2002). Kinesiology of the Musculoskeletal System. St. Louis: Mosby.
A second set of connective tissue pulleys called cruciate pulleys give additional support and stability to the tendon sheaths. The term cruciate means cross and you can see by their structure where they get their name (Figure 1). The cruciate pulleys are much smaller than the annular pulleys. There are three cruciate pulleys, designated as C1, C2, and C3. Their role for improving the flexor tendon’s angle of pull is not as great, so if they are damaged, finger movement is not impaired as much.
The annular pulleys may be damaged from an acute injury or from various degenerative conditions in the fingers. An example of the detrimental effect of rupture of the annular pulleys is shown in Figure 3. In this image, the A3 pulley has been completely ruptured and there is a partial rupture to the A2 pulley. As a result, the tendon is pulled away from the PIP joint in what is referred to as a bowstringing effect. With the tendon pulled away from the PIP joint, its power is reduced and it is no longer able to produce normal range of motion. As a result, the hand is significantly weaker in gripping activities.
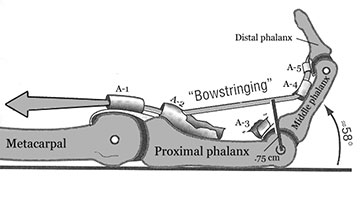
Figure 3: Injury to the flexor pulleys
From Neumann, D. A. (2002). Kinesiology of the Musculoskeletal System. St. Louis: Mosby.
Stenosing tenosynovitis, also called trigger finger, is another disorder involving the flexor pulleys. In this condition, a fibrous nodule develops on the tendon near the edge of the tendon sheath. The nodule prevents the tendon from freely gliding in and out of the surrounding synovial sheath. Stenosing tenosynovitis is usually a problem with the tendon sheath, but in some cases the nodule on the tendon catches on the edge of the flexor pulleys. If this is the case, the offending flexor pulley can be surgically cut to allow the tendon greater freedom of movement. However, if the pulley has been cut, that flexor tendon is less efficient so the benefits of this procedure need to be weighed against the potential drawbacks.
While massage practitioners may not see a large number of clients with flexor pulley dysfunctions, there is still great value in understanding these details of hand mechanics. After all, the hand is our primary tool that we use in our work as soft-tissue therapists, and we need to keep it in good condition. Overuse problems may affect our ability to keep working, and physical injury is one of the primary reasons people leave this profession, understanding more about proper mechanics helps keep you in better condition.
- Neumann, D. A. Kinesiology of the Musculoskeletal System. St. Louis: Mosby, 2002
This article originally appeared in Massage Today.
